Understanding Obesity and the Benefits of Weight Loss Surgery
Obesity is a complex and chronic medical condition affecting millions of Australians. It is increasingly recognised as a disease — not simply a lifestyle issue — and often requires more than diet and exercise alone to manage effectively.
At its simplest, obesity is defined as:
“A condition characterised by excessive accumulation of body fat, typically indicated in adults by a body mass index (BMI) of 30 or greater.”
But in reality, obesity is far more complex — and so is its treatment.
Key Takeaways
How does obesity affect the body beyond weight gain?
Obesity impacts multiple body systems by increasing inflammation, disrupting hormones, and placing strain on the heart, joints, and metabolic function.
Why is obesity considered a chronic disease rather than just a lifestyle issue?
Obesity is recognised as a chronic condition because it involves complex biological, genetic, and hormonal drivers that make long-term weight regulation difficult.
What role do hormones play in weight gain and weight loss?
Hormones that regulate hunger, fullness, and metabolism can make it harder to lose weight and easier to regain it after dieting.
How does weight loss surgery influence appetite and hunger?
Weight loss surgery alters hunger hormones, helping reduce appetite and improve feelings of fullness after smaller meals.
What makes surgical weight loss more effective long term for some patients?
Surgery addresses both physical restriction and hormonal factors, leading to more sustainable weight loss compared to lifestyle changes alone.
How quickly do patients typically see results after weight loss surgery?
Most patients begin losing weight rapidly in the first few months, with continued progress over 12–18 months.
Can weight loss surgery improve overall quality of life?
Yes, many patients experience increased mobility, improved energy levels, and better mental wellbeing following significant weight loss.
Is weight loss surgery a standalone solution?
No, long-term success requires ongoing lifestyle changes including nutrition, physical activity, and follow-up care.

What Is Obesity?
Obesity is a chronic medical condition defined by an excessive accumulation of body fat, typically indicated by a body mass index (BMI) of 30 or higher. It is influenced by genetic, hormonal, environmental, and lifestyle factors, and increases the risk of conditions such as type 2 diabetes, heart disease, and certain cancers.
What BMI Is Considered Obese?
In adults, a BMI of 30 or higher is classified as obese.
- 25–30: Overweight
- 30–35: Obese
- 35–40: Severely obese
- 40+: Morbidly obese
BMI is a useful screening tool, but a full medical assessment is important. Check your BMI eligibility.
Understanding Obesity: A Chronic Medical Condition
Obesity develops when there is a long-term imbalance between energy intake and energy expenditure. However, this is influenced by multiple factors, including:
- Genetics
- Hormonal regulation
- Dietary patterns
- Physical activity
- Medical conditions and medications
- Environmental and psychological factors
Obesity is now recognised as a chronic, systemic condition affecting overall health.

How Is Obesity Measured?
Body Mass Index (BMI) is the most commonly used screening tool.
BMI Categories for Adults
- Healthy weight: 20 – 25
- Overweight: 25 – 30
- Obese: 30 – 35
- Severely obese: 35 – 40
- Morbidly obese: 40+
BMI is a guide only — individual assessment is essential.
Obesity in Australia: A Major Health Issue
Obesity is one of the leading contributors to disease burden in Australia.
- Around two-thirds of Australian adults are overweight or obese
- Rates have increased significantly over time
- Millions meet criteria for medical or surgical treatment
Despite this, many eligible patients do not access effective treatment options.
Some key Australian obesity statistics*:
- Almost 2 in 3 Australian adults were overweight or obese in 2014-2015
- 28% of Australian adults were obese in 2014-2015, an increase from 19% in 1995
- 1 in 4 Australian children (aged 2-17) were overweight or obese in 2014-2015
- In 2014-2015 there were 22,700 hospital admissions for weight loss surgery in Australia (more than double that of 2005-06 – about 9,300)
- In 2017-18, the Australian Bureau of Statistics’ National Health Survey showed that two thirds (67.0%) of Australian adults were overweight or obese (12.5 million people), an increase from 63.4% in 2014-15. The National Health Survey also indicated that almost one quarter (24.9%) of children aged 5-17 years were overweight or obese in 2017-18 (17% overweight and 8.1% obese).
Health Risks Associated with Obesity
Obesity increases the risk of:
- Type 2 diabetes
- Cardiovascular disease
- High blood pressure
- Sleep apnoea
- Joint problems
- Reflux (GORD)
- Certain cancers
As weight increases, so does the risk.
Why Weight Loss Is So Difficult to Maintain
Many people experience short-term success with diet and exercise, followed by weight regain.
This is not simply a lack of discipline.
The body actively resists weight loss through:
- Slowing metabolism
- Increasing hunger hormones
- Reducing satiety signals
This makes sustained weight loss difficult without medical support.
Weight Loss Surgery
Common types of weight loss procedures include:
Each procedure is tailored to the individual.
How Weight Loss Surgery Works
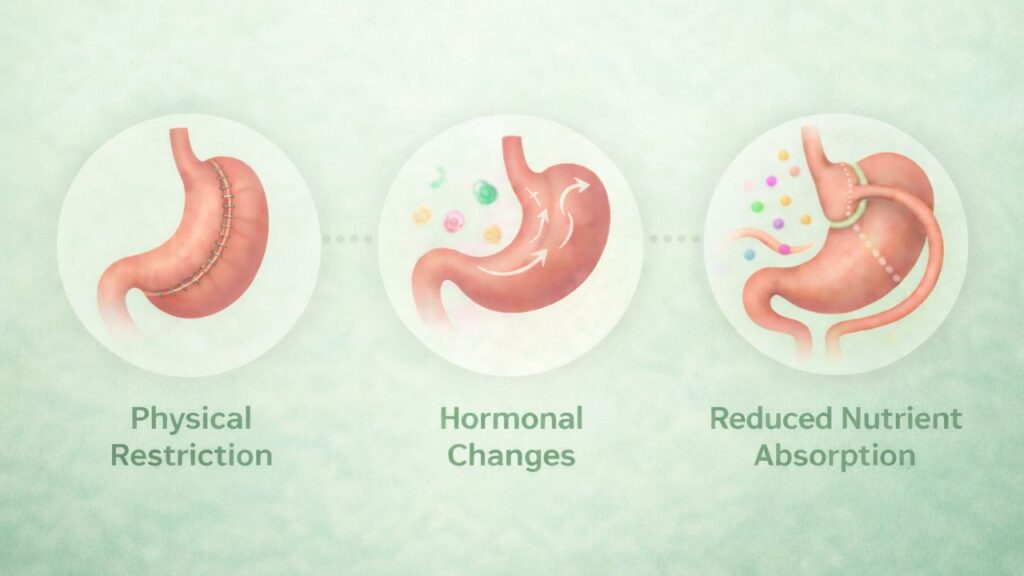
Weight loss (bariatric) surgery is widely recognised as the most effective long-term treatment for obesity.
It works through three key mechanisms:
1. Physical Restriction
A smaller stomach means smaller meals are needed to feel full.
2. Hormonal Changes
Changes in gut hormones reduce hunger, improve fullness, and help regulate blood sugar.
3. Reduced Nutrient Absorption (in some procedures)
In procedures such as gastric bypass, part of the small intestine is bypassed, which:
- Reduces calorie absorption
- Changes how nutrients are absorbed
- Enhances weight loss and metabolic outcomes
Because of this, ongoing nutritional monitoring is essential.

How Effective Is Weight Loss Surgery?
Weight loss surgery delivers strong and sustained results:
- 25–30% total body weight loss within the first year
- Long-term weight maintenance
- Improvement or remission of obesity-related conditions
Is Weight Loss Surgery Safe?
Modern weight loss surgery is safe and well-established when performed by experienced surgical teams, with low complication rates.
Is Weight Loss Surgery Right for You?
You may be a candidate if:
- Your BMI is 35 or higher, or
- Your BMI is 30–34 with obesity-related conditions
A full assessment is required to determine suitability.

Taking the First Step to Weight Loss
Obesity is a complex condition — but effective treatments are available.
Weight loss surgery offers:
- Significant and sustained weight loss
- Improved overall health
- Long-term quality of life benefits
Start Your Journey Today
👉 If you’re considering weight loss surgery, the first step is a consultation to understand your options.
Obesity and Weight Loss Surgery FAQs
What causes obesity?
Obesity is caused by a combination of genetic, hormonal, environmental, and lifestyle factors. It is a chronic medical condition, not simply a result of diet alone.
Can obesity be treated without surgery?
Yes. Lifestyle changes are important, but long-term weight loss is often difficult to maintain. Medical or surgical treatment may be recommended.
Who is eligible for weight loss surgery?
Patients with BMI ≥ 35, or BMI 30–34 with obesity-related conditions, may be eligible.
What is the difference between gastric sleeve and gastric bypass?
Gastric sleeve reduces stomach size and affects hunger hormones.
Gastric bypass also changes the digestive tract, reducing nutrient absorption and often producing stronger metabolic effects.
How much weight can you lose after surgery?
Most patients lose 50–70% of excess body weight, depending on the procedure.
Will I need vitamins after weight loss surgery?
Yes. All patients require vitamin and protein supplementation after weight loss surgery to support healing, maintain nutrition, and preserve muscle mass.
Patients who undergo gastric bypass typically require more intensive and long-term supplementation, as nutrient absorption is reduced.
How long does recovery take?
Most patients return to normal activities within 2–4 weeks, depending on the procedure.
Is weight regain possible after surgery?
Some weight regain can occur over time, but surgery provides long-term tools to help maintain weight loss when combined with lifestyle changes and ongoing support.
*Statistics Source
Australian Government, Australian Institute of Health and Welfare
https://www.aihw.gov.au/reports-statistics/behaviours-risk-factors/overweight-obesity/overview
https://www.aihw.gov.au/reports-statistics/behaviours-risk-factors/overweight-obesity/about
Australian Government, Department of Health
http://www.health.gov.au/internet/main/publishing.nsf/Content/Overweight-and-Obesity







